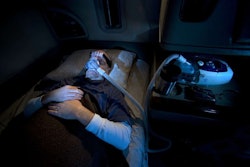
Driver Scott LeVan of Watsontown, Pa., recently went to the Concentra clinic in Wilkes-Barre, Pa., for his regular U.S. Department of Transportation-required physical to renew his medical certification.
“I passed everything,” LeVan said. But the examiner, citing LeVan’s body mass index (BMI) measurement over 32 and a history of high blood pressure, said: “I’m going to hold your certification.”
The issue was the possibility that LeVan had sleep apnea. It’s a disqualifying condition under the medical rules if reaching a severity that affects daytime sleepiness and is left untreated. Nothing new there, but the examiner didn’t issue a conditional certification for LeVan so that he at least could continue working while it was determined via an in-lab sleep study whether he suffered from the condition or not.
LeVan says the examiner and others at the clinic stressed that federal rules required the test based on those specific BMI criteria, as well as the hold on his certification, until he received results of a sleep study. If it was negative for apnea, he could get his certification. If positive, treatment would need to begin before his certification could be issued.
Report: How to address sleep apnea risk on your own terms.
LeVan is not the only driver to find new emphasis being placed on apnea screening and tests during their most recent certification. Nor is he alone in being taken off the road indefinitely simply because he’s considered at-risk for the condition. With federal regulations regarding the condition long in limbo and several sets of cases that actually contradict federal panel-issued guidance available for examiners to consult, knowing what to expect from apnea screening has grown more difficult. Drivers who suspect they may be at risk (see the how-to on assessing risk at this link) would be advised to get out ahead of the issue by settling their diagnosis outside of the medical certification process.
One in five respondents to the following Overdrive poll conducted in June said their most recent certification resulted in apnea testing and/or treatment. Half of that 20 percent said no temporary certification – an option available to the examiner at his or her discretion – was issued to bridge the gap and keep the driver rolling during the time it took to test and treat.
When LeVan spoke with Overdrive in June, he was $2,000 in arrears considering downtime, lost pay and associated expenses.
What’s in the regulations on sleep apnea?
Very little, notes Federal Motor Carrier Safety Administration spokeswoman Marissa Padilla.
The condition is mentioned in Title 49 of the Code of Federal Regulations, section 391.41(b)(5):
A person is physically qualified to drive a commercial motor vehicle if that person: Has no established medical history or clinical diagnosis of a respiratory dysfunction likely to interfere with ability to control and drive a commercial motor vehicle safely.
Since a driver must be alert at all times, any change in his or her mental state is in direct conflict with highway safety. Even the slightest impairment in respiratory function under emergency conditions (when greater oxygen supply is necessary for performance) may be detrimental to safe driving. There are many conditions that interfere with oxygen exchange and may result in incapacitation, including emphysema, chronic asthma, carcinoma, tuberculosis, chronic bronchitis and sleep apnea.
The regulation goes on to state that if examiners detect “a respiratory dysfunction that in any way is likely to interfere with a driver’s ability to safely control and drive a commercial motor vehicle, the driver must be referred to a specialist for further evaluation and therapy.”
|
DOES FMCSA PLAN TO PURSUE A RULEMAKING RELATIVE TO SLEEP APNEA TESTING AND TREATMENT? That’s from agency spokesperson Marissa Padilla, though the issue is not on DOT’s regulatory calendar as of the most recent publication, and recently former Administrator Anne Ferro said in a relatively recent congressional hearing that there were no near-term plans for a rule. Padilla emphasizes, however, that following 2013 legislation Congress passed to require “FMCSA to address any further guidance on obstructive sleep apnea through the formal rulemaking process,” the agency will pursue such a rulemaking. |
There is likewise no official regulatory guidance on the subject, either, though in 2012 the agency accidentally released – and later retracted – what appeared to be a proposal to adopt official guidance. It hewed closely to recommendations issued by a joint meeting of the agency’s Medical Review Board of doctors and the Motor Carrier Safety Advisory Committee.
Those recommendations, however, continue to be in the less-official realm of general guidance. That’s a distinction many medical examiners don’t understand, says driver Bob Stanton, cofounder of Truckers for a Cause, a sleep apnea support group and a chapter of the American Sleep Apnea Association’s A.W.A.K.E. organization.
Stanton defines regulatory guidance as where “FMCSA has officially adopted recommendations of outside medical groups or advisory panels and incorporated it in the instruction.” He uses the somewhat clear-cut blood-pressure guidance as an example.
With general guidance, however, “the medical examiner is supposed to use his own best professional judgment on how to apply it,” says Stanton. To date, there have been three different sets of this sort of guidance on screening for sleep apnea from federally convened boards and panels.
The first, in 2006, specified a set of seven procedures. A 2008 Medical Expert Panel specified a BMI greater than 33, among other factors such as neck size and various questionnaires. The 2012 joint recommendations from the MRB/MCSAC joint meeting took the BMI recommendation higher to 35, again among other considerations.
So not only has FMCSA failed to specify exactly what approach a medical examiner has to take regarding apnea, there exist three different “general guidance” standards for an examiner to interpret under his own judgment.
Why are doctors now more aggressive on apnea?
Two answers: One has to do with new training all docs giving DOT physicals have been required to take. The other has to do with liability.
 Dr. Randolph Rosarion shares insights on being a U.S. Department of Transportation medical examiner and other issues via his Dotmedicalexaminer.com website.
Dr. Randolph Rosarion shares insights on being a U.S. Department of Transportation medical examiner and other issues via his Dotmedicalexaminer.com website.Dr. Randolph Rosarion, based in College Point, N.Y., says his sleep apnea referrals are far less than two in 10 drivers he sees for testing. Rosarion says he relies not only on BMI measurement but also on sleep habits and reporting of episodes of daytime sleepiness. Add in diabetes and/or high blood pressure as contributing factors, and the driver’s condition may rise to the level where Rosarion would refer him “to a pulmonary specialist who practices sleep medicine,” he says, as required in the regulations.
If the driver has insurance, it usually covers the visit and any subsequent test in a sleep lab or using a portable unit at home – a less-expensive option that in some ways is more appealing. In others, not so much, speculates Rosarion, given less-than-ideal diagnostic capabilities: “I prefer to send the person to a sleep expert and have them evaluated with a formal sleep study” in a lab.
Rosarion says congressional attention to apnea with last year’s legislation raised awareness in the medical community and among drivers about the condition. That legislation pulled back the reins on FMCSA’s piecemeal approach by requiring that any new apnea regulation go through a formal rulemaking.
In addition, the National Registry of Certified Medical Examiners’ institution this year has been reinforcing a lot of the guidance that exists on the condition, Stanton notes. “The actual training that the medical examiners must get to be certified [and listed in] the National Registry is not administered by FMCSA,” he says. It’s administered by outside training organizations, per FMCSA’s guidance, so the exact training materials that a medical examiner gets may vary, he says.
Stanton says this variability is problematic, given the difficulty to access documents to determine what guidance on apnea is being taught and thus how to advise a particular driver.
Last May, the registry finally went live, requiring drivers to use only examiners listed within it. During Rosarion’s December 2012 training, guidance for apnea screening specified 33 as a BMI cutoff, above which drivers should be considered at-risk.
“There are pretty clear guidelines,” he says, which originate with FMCSA’s 2008 Medical Expert Panel recommendations. The patient’s “neck size is also a risk factor – a 17-inch [or larger] neck for a guy, 16 for a woman.”
But in documents obtained by Overdrive from a medical examiner who wished to remain anonymous, another set of training materials hews more closely to the MRB/MCSAC’s joint recommendations issued in early 2012, specifying the BMI cutoff at 35. Crucially, the procedure outlined in these documents called for a one-month waiting period for a driver treated with the most common method, a continuous positive airway pressure (CPAP) machine, and longer for those treated surgically. No conditional short-term temporary certification is specified as an option to examiners.
An agency official speaking on background noted that FMCSA’s brief eight-page guidance on the training curriculum has only a few references to sleep apnea. On its page listing organizations providing training to be certified for the NRCME, FMCSA washes its hands of the actual content of the training with a disclaimer: “It is the responsibility of the medical examiner applicant to determine if the training provided by an organization meets the requirements of FMCSA’s regulations.”
Q: Can an employer fire or refuse to hire me on account of a sleep apnea diagnosis?
With no clear-cut approach to screening and treatment, many examiners, says Stanton, err on the side of caution. “Medical examiners are scared about their liability exposure in the event of a driver they did an exam on later being involved in an accident where sleep apnea was a contributing causal factor,” says Stanton, referencing rumors of cases settled out of court with no public documentation. “The problem is until a case goes to trial and there’s some public clarification of an examiner’s liability exposure and FMCSA is able to set standards, the medical examiners are trying to cover their anatomy.”
That means more testing, at more expense to drivers, with increased chances of being taken off the road before a diagnosis is reached.
At once, as LeVan’s case illustrates, for those who truly are suffering from apnea, a silver lining to the rigamarole that many have been going through during certification exists. Following up with LeVan in August, the driver noted he was back up and running with his carrier and that CPAP treatment was proceeding well. Ultimately, “I’m glad I did get tested,” he says. “I feel much better – just all around feel great. So maybe this was an awakening for me.”