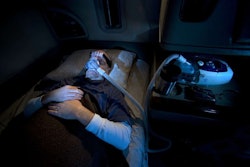
Sleep-apnea-related federal listening sessions are fast approaching. The first is next week in Washington, D.C., and all are part of the Federal Motor Carrier Safety Administration’s information/perspective-gathering expedition as it contemplates potential rulemaking relative to the sleep apnea condition’s presence in medical certification processes for truck operators.
The sessions, in downtown Washington, D.C.; Chicago, Ill.; and Los Angeles May 12, 17 and 25, respectively, are not in locales that are particularly truck-friendly, and no convenient truck parking is available.
Nonetheless, for those with an interest in attending and commenting on the incidence, prevalence, treament of and safety relevance of sleep apnea, among other related topics, trucker Bob Stanton of the Truckers for a Cause sleep apnea patient support group has compiled information from drivers familiar with each area — and, in the case of the D.C. meeting, from the Owner-Operator Independent Drivers Association.
You can find a wealth of information for each meeting location at the Truckers for a Cause website via this link. There is likewise a Share a Ride sign-up option on the site.
Driver Stanton and company have also put together a Facebook group accessible at this link to allow drivers to exchange information on ride, taxi or Uber sharing.
As previously reported, each listening session is open to the public, and the FMCSA has asked that speakers limit their comments to 3-5 minutes. In preparing your comments, review the 20 questions FMCSA posted to help guide you through the kinds of perspectives the agency is looking for — while some might not apply directly to drivers, many do, and drivers’ experiences with the condition in medical certifications in recent years are germane to the discussion.
You can find the questions at this link with further explanatory text — and listed by themselves at the bottom of this story.
Those who cannot attend the meeting in person can view a live webcast and will be given a chance to submit comments online that will be read aloud at the sessions. FMCSA will post specific information on how to participate via the webcast at this link to the agency’s calendar page ahead of the sessions. And whether you can attend in person or via the webcast or not, the comment period on the initial Advance Notice of Proposed Rulemaking remains open through June 8.
Drivers interested in commenting, through the June 8 deadline, can do so directly via this link to Regulations.gov.
The 20 questions in FMCSA’s sleep apnea ANPRM
1. What is the prevalence of moderate-to-severe Obstructive Sleep Apnea (OSA) among the general adult U.S. population? How does this prevalence vary by age?
2. What is prevalence of moderate-to-severe OSA among individuals occupying safety sensitive transportation positions? If it differs from that among the general population, why does it appear to do so? If no existing estimates exist, what methods and information sources can the Agencies use to reliably estimate this prevalence?
3. Is there information (studies, data, etc.) available for estimating the future consequences resulting from individuals with OSA occupying safety sensitive transportation positions in the absence of new restrictions? For example, does any organization track the number of historical motor carrier or train accidents caused by OSA? With respect to rail, how would any OSA regulations and the current positive train control system requirements interrelate?
4. Which categories of transportation workers with safety sensitive duties should be required to undergo screening for OSA? On what basis did you identify those workers?
5. What alternative forms and degrees of restriction could FMCSA and the Federal Railroad Administration (FRA) place on the performance of safety-sensitive duties by transportation workers with moderate-to-severe OSA, and how effective would these restrictions be in improving transportation safety? Should any regulations differentiate requirements for patients with moderate, as opposed to severe, OSA?
6. What are the potential costs of alternative FMCSA/FRA regulatory actions that would restrict the safety sensitive activities of transportation workers diagnosed with moderate-to-severe OSA? Who would incur those costs? What are the benefits of such actions and who would realize them?
7. What are the potential improved health outcomes for individuals occupying safety sensitive transportation positions who would receive OSA treatment due to regulations?
8. What models or empirical evidence is available to use to estimate potential costs and benefits of alternative restrictions?
9. What costs would be imposed on transportation workers with safety sensitive duties by requiring screening, evaluation, and treatment of OSA?
10. Are there any private or governmental sources of financial assistance? Would health insurance cover costs for screening and/or treatment of OSA?
11. What medical guidelines, other than those the American Academy of Sleep Medicine guidance the Federal Aviation Administration currently uses, are suitable for screening transportation workers with safety sensitive duties that are regulated by FMCSA/FRA for OSA? What level of effectiveness are you seeing with these guidelines?
12. What were the safety performance histories of transportation workers with safety sensitive duties who were diagnosed with moderate-to-severe OSA, who are now successfully compliant with treatment before and after their diagnosis?
13. When and how frequently should transportation workers with safety sensitive duties be screened for OSA? What methods (laboratory, at-home, split, etc.) of diagnosing OSA are appropriate and why?
14. What, if any, restrictions or prohibitions should there be on transportation workers’ safety sensitive duties while they are being evaluated for moderate-to-severe OSA?
15. What methods are currently employed for providing training or other informational materials about OSA to transportation workers with safety sensitive duties? How effective are these methods at identifying workers with OSA?
16. What qualifications or credentials are necessary for a medical practitioner who performs OSA screening? What qualifications or credentials are necessary for a medical practitioner who performs the diagnosis and treatment of OSA?
17. With respect to FRA, should it use Railroad MEs to perform OSA screening, diagnosis, and treatment?
18. Should MEs or Agencies’ other designated medical practitioners impose restrictions on a transportation worker with safety sensitive duties who self-reports experiencing excessive sleepiness while performing safety sensitive duties?
19. What should be the acceptable criteria for evaluating the effectiveness of prescribed treatments for moderate-to-severe OSA?
20. What measures should be used to evaluate whether transportation employees with safety sensitive duties are receiving effective OSA treatment?