Being referred for sleep apnea screening can be an expensive requirement for truck operators, particularly for those without health insurance, according to new research released May 26 by the American Transportation Research Institute. Costs to truckers many times exceed $1,000 in out-of-pocket expenses, according to ATRI’s study.
The report comes the day following the conclusion of the third and final federal listening session relative to pursuit of a potential sleep apnea rulemaking by the U.S. DOT.
ATRI based its report on results of a survey of drivers around issues related to the obstructive sleep apnea (OSA) condition. Based on the responses of more than 800 drivers (7 in 10 of them company employee drivers, the balance owner-operators), conclusions underscore a number of the issues raised during the listening sessions relative to the costs, incidence and effectiveness of screening and testing for and treatment of sleep apnea.
ATRI’s report attempts to quantify the costs and other impacts that truck drivers are experiencing as they address a diagnosis and potential treatment regimen for OSA.
“ATRI’s research clearly shows what my fellow drivers and I have been experiencing,” said owner-operator Barbara Beal. “The costs associated with sleep apnea screening and treatment are not inconsequential for drivers and the flexibility to utilize lower cost options for both screening and treatment will be critical if FMCSA moves forward with a formal rulemaking.”
Incidence of screening, testing and treatment has risen in recent years among drivers. Recent polling here at OverdriveOnline.com showed a more than 10 percentage-point increase in the number of drivers reporting having been tested for apnea.
Have you been tested/treated for sleep apnea?
Two years back, the last time that question was asked directly to Overdrive readers, more than 60 percent of responded in the No column, lending credence to anecdotal evidence that the willingness of examiners to refer drivers for testing is indeed on the rise. The variability of screening protocols for apnea test referrals has been perhaps the biggest point of contention among critics of how the medical certification process treats the condition today. The ATRI survey found that, among both drivers who have had sleep studies and those who have not, there is concern about the use of neck circumference and Body Mass Index (BMI) as measures to refer drivers to sleep studies.
Additionally, among drivers who have been tested, 64 percent believe that the DOT guidelines for referring drivers are too broad and that medical examiners do not follow the guidelines for referrals to sleep studies.
COSTS
Going through the testing-referral process can be a costly proposition, ATRI’s study finds.
Among drivers who had been referred for a sleep study, 53 percent paid some or all of the test costs, with an average of $1,220 in out-of-pocket expenses, representing just more than 1.5 weeks of median driver pay at $805 per week, the survey authors note.
Meanwhile, health insurance assistance with sleep study costs impacted driver out-of-pocket costs significantly — 61 percent of drivers with no health care coverage of their sleep study incurred out-of-pocket costs exceeding $1,000. At the same time, 32 percent of drivers whose health insurance did cover some portion of the sleep study reported costs exceeding $1,000.
Among drivers reporting time away from work associated with sleep apnea screening, 41 percent indicated days off ranging from 1-30 days.
TREATMENT
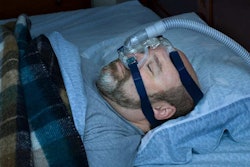
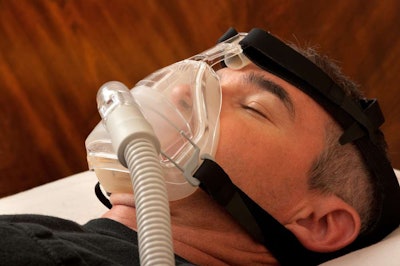
Use of a Continuous Positive Airway Pressure (CPAP) machine was the most commonly reported prescribed treatment regimen for drivers diagnosed with sleep apnea. This includes drivers in the ATRI sample diagnosed with mild sleep apnea, a condition that — though as noted above practices among medical examiners have been notoriously variable — ATRI says does not require treatment for medical certification.
The number of drivers who report not adhering to a prescribed OSA treatment was a scant 1.95 percent of the moderate/severe OSA-diagnosed respondents, the survey report stresses, underscoring well-known health/lifestyle benefits of treatment for those who truly suffer from the condition.
Along similar lines, drivers’ perception of treatment efficacy varied by sleep apnea severity. As OSA diagnosis severity increased, drivers experienced more positive CPAP treatment effects. For example, drivers diagnosed with severe OSA and being treated with CPAP reported increased amounts of sleep (84 percent), feeling better when they wake up (71 percent), and lower blood pressure (75 percent).
Downloads of the full survey report are available via this link to ATRI’s website.
Conversely, of the 91 percent of drivers being treated with CPAP — despite a diagnosis of mild sleep apnea — less than a third (32 percent) experienced improved sleep as a result of CPAP treatment.
The comment period for FMCSA’s fact-finding Advanced Notice of Proposed Rulemaking on sleep apnea is open through June 8. Drivers interested in commenting can do so directly via this link to Regulations.gov. You’ll 20 specific questions the agency asked relative to apnea in this post from early May.